Hypothyroidism is a leading cause of difficulty in achieving and maintaining pregnancy. Low thyroid function has a negative impact on reproductive health and is more common than most women realize. In this guide we’ll be discussing thyroid imbalances and their effects on fertility and pregnancy, proper nutrition for hypothyroidism, and the 12 most effective herbs to help support the thyroid including fertility super herbs vitex and maca root.
In the ever-changing medical system, new information on thyroid testing has narrowed the ranges in which thyroid function impacts a woman’s ability to achieve pregnancy. For women struggling to get pregnant, questioning thyroid health and getting proper testing is a first critical step to a successful outcome.
Fortunately, for the thousands of women that are diagnosed with hypothyroidism, there are a variety of natural ways to support thyroid health. Along with your doctor monitoring thyroid hormone levels and prescribing thyroid medication, there are specific foods, key nutrients and herbs that can all be used to improve thyroid health. The thyroid is a key link to whole body wellness.
Get to Know The Thyroid
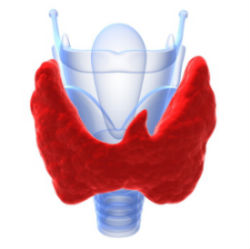
The thyroid gland is a butterfly shaped gland that partially surrounds the wind pipe. The thyroid produces thyroid hormones, mainly thyroxine (T4) and small amounts of triiodothyronine (T3). T3 is the more active form of thyroid hormone that tells cells what to do, and T4 is converted into T3 inside the target cells.
What thyroid hormones do:
- Control metabolism by regulating the rate of oxygen consumption and consequent heat production at the cellular level.
- Influence carbohydrate, protein and fat metabolism.
- During pregnancy, fetal growth and development are controlled by maternal thyroid hormone, with the help from fetal thyroid hormone later in pregnancy. Growth and development continue to be regulated by the thyroid postpartum.
- Healthy thyroid function is also required for the activity of other hormones, like growth hormone, for controlling heart rate and blood pressure, and even for proper brain function.

Learn How To Support Your Thyroid Naturally With My Thyroid Mini-Course
- Learn how to support your thyroid naturally with nutrition, supplements and plants.
- Know how to tell whether your thyroid, endocrine system or/and adrenals needs support
- Self-care therapies to support your thyroid and endocrine system
The Bigger Picture – The Thyroid and the Endocrine System
The thyroid is part of the endocrine (hormonal) system and is controlled by the hypothalamus and the pituitary gland in the brain. To understand the role the thyroid plays as an endocrine gland, let me break it down into the cycle of communication that takes place…
➞ The hypothalamus produces Thyrotropin Releasing Hormone (TRH), which tells the pituitary gland to make Thyroid Stimulating Hormone (TSH).
➞ TSH tells the thyroid to make thyroid hormone, which is then carried to the target cells by Thyroxine Binding Globulin (TBG). Thyroid hormone that is bound to TBG is inactive until released and entering the target cell.
➞ Importantly, thyroid hormone regulates its own production by telling the pituitary to reduce production of TSH in a “negative feedback loop”.
You may recognize TSH from your lab test, as it’s commonly used to measure thyroid activity. As confusing as all this may sound, the more thyroid hormone there is, the lower TSH levels will be. The lower thyroid hormone is, the higher TSH will be (usually!).
Doctors use high and low TSH to diagnose hypothyroidism (low functioning thyroid) and hyperthyroidism (over-functioning thyroid), respectively. However, reliance of TSH levels alone in diagnosing thyroid issues gives an incomplete and potentially misleading picture (more on this later).
A Delicate Balance – Endocrine Glands & Hormonal Balance
Also under control of the hypothalamus and pituitary gland are the ovaries and adrenal glands. In response to Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH) produced by the pituitary, the ovaries produce estrogen and progesterone. In response to Adrenocorticotropic Hormone secreted by the pituitary, the adrenals make cortisol (“stress hormone”). A similar negative feedback loop exists between ovarian and adrenal hormones and the hypothalamus and pituitary, just like with thyroid hormone.
You can think of all of these glands — hypothalamus, pituitary, thyroid, ovaries, adrenals — as being a part of a spider’s web. When something happens at one part of the web, it’s felt through the entire web. Thus, imbalances anywhere in this system will influence the other glands and hormones in the system.
Hypothyroidism
When thyroid function is not sufficient to meet the body’s needs it is called hypothyroidism, and may stem from various sources…
➞ For one, the thyroid may not make enough of the T4 form of thyroid hormone due to a problem with the thyroid itself. In this case, T4 levels would be low and TSH would be high because there wouldn’t be enough T4 to inhibit the pituitary’s production of TSH in the negative feedback loop. Hashimoto’s Disease is an example of this in which the thyroid can’t keep up with the body’s needs because it is being targeted by the immune system for destruction (“autoimmunity”).
➞ Iodine deficiency is another cause of hypothyroidism, because iodine is necessary for production of thyroid hormone. (T4 has 4 iodides and T3 has 3.)
➞ Another reason T4 might not be made is due to problems upstream with the hypothalamus and/or pituitary. In this case, both T4 and TSH may both be low.
➞ Alternatively, there may be plenty of T4 made by the thyroid, but it is not being converted to the more active T3 in target cells. In this case, T4 and TSH levels may look fairly normal, but T3 will be lower than usual. Yet another issue may be that T4 is being converted into an inactive form of T3 known as reverse T3 (rT3). Again, T4 and TSH may appear relatively normal in this case.
Signs of Low Thyroid Function
If you have more than three of the following signs, consider having your thyroid tested:
- Fatigue, weakness
- Depression, irritability
- Mind fog, memory loss
- Digestive issues – usually constipation/slow food transit (can measure this via the beet test!)
- Weight gain or difficulty losing weight
- Dry/rough skin, dry/brittle hair, hair loss
- Eczema
- Shortness of breath
- Cold intolerance
- Low body temperature
- Slow pulse
- Goiter (swollen thyroid)
- Muscle cramps
- Reduced libido
- Menstrual cycle abnormalities
- Difficulty conceiving or carrying pregnancy
Click here to learn more about a nutritional and herbal supplement for thyroid health…
New Thyroid Testing Guidelines
The Importance of Complete Thyroid Hormone Testing
Many doctors only measure TSH, or TSH and T4 as recommended by the American Thyroid Association. This means that you may have symptoms of hypothyroidism and are told that your thyroid function is normal, when in fact there may be problems such as poor T4-to-T3 conversion or high levels of rT3 that wouldn’t be uncovered without additional tests. When having thyroid function checked, a more comprehensive approach would be to assess TSH, total T4 (T4 bound or not bound to TBG), free T4 (T4 not bound to TGB), total T3, and free T3. rT3, if available, should also be included, as well as tests for the presence of thyroid autoantibodies.
Understanding TSH Levels to Diagnose Hypothyroidism
Today experts consider 0.3 to 3.0 mIU/L the normal range for TSH levels to fall (14). Anything above 3.0 is considered hypothyroid. Some endocrinologists believe that a percentage of women may find it difficult to get pregnant — or maintain a pregnancy — at a TSH level above 2.0 mIU/L, which may indicate poor thyroid function. Some studies indicate that TSH levels should be below 2.5 mIU/L prior to conception, while other studies suggest it should be at or below 1.2 mIU/L as shared by the American Thyroid Association.
Thyroid Monitoring is Imperative to a Healthy Pregnancy
Along these lines, The American Thyroid Association has released new TSH and T4 testing guidelines for pregnant women, based on trimester. For the first trimester, the normal TSH range is 0.1-2.5 mIU/L, for the second it’s 0.2-3mIU/L and for the third it’s 0.2-3.0 mIU/L. For comparison, the normal range for women who are not pregnant used to be 0.4-4.0 mIU/L, which was considered the normal range for both pregnant and nonpregnant women. Overt hypothyroidism is now defined in pregnancy as either (i) TSH levels greater than 2.5mIU/L and decreased free T4 or (ii) TSH levels greater than 10mIU/L regardless of free T4 levels. Subclinical hypothyroidism is now defined in pregnancy as TSH levels between 2.5 and 10mIU/L and normal free T4 levels.
Reproductive Hormones & Medications Impact Thyroid Health
Thyroid function influences reproductive hormone balance, but reproductive hormones also influence thyroid function. High levels of estrogen, whether due to estrogen dominance or taking exogenous estrogen, may reduce the amount of active thyroid hormone. This is because excess estrogen increases TBG, the protein that binds and transports T4 and T3 but also renders them inactive upon binding. In those with normal thyroid function, a compensatory increase in thyroid hormone takes care of this but in hypothyroid women, this compensation doesn’t happen and symptoms of hypothyroidism may worsen in the presence of excess estrogen (New England Journal of Medicine).
Finally, many prescription medications also block thyroid function, including steroids, beta-blockers, barbiturates, cholesterol-lowering drugs, and certain seizure medications. If you are experiencing signs of low thyroid function, be sure to research any medications you are taking to look for impacts on the thyroid.
Hypothyroidism, Fertility and Pregnancy
Fertility & Conception
Conception is more difficult for hypothyroid women due to associated ovarian dysfunction (remember the spiderweb analogy). Both hypo- and hyperthyroidism disrupt reproductive hormone balance and women with thyroid disorders often have menstrual cycle abnormalities such as flooding, scanty periods or irregular cycles. While the precise mechanisms of hormonal disruption have yet to be defined, research in The Journal of Obstetrics and Gynecology of India shows hypothyroidism has been associated with reduced FSH and LH levels which are needed for egg follicle maturation and ovarian production of estrogen and progesterone. Hypothyroidism has also been linked with the development of ovarian cysts, and such cysts may regress upon thyroid treatment (Journal of Pediatric Endocrinology and Metabolism, 2011).
Pregnancy
It is not uncommon for thyroid disorders to develop during pregnancy, with an incidence ranging from 10-15%. Thyroid hormone is important for both placental and fetal development. Pregnancy can be seen as a “stress test” for the thyroid in that the mother’s thyroid hormone production needs to increase by 20-50% to accommodate the increased metabolic needs of mother and developing fetus. If a woman is unable to produce enough thyroid hormone due to overt (“full blown”) hypothyroidism, or even to subclinical hypothyroidism then that becomes a problem under the increased demands of pregnancy, the risk of miscarriage, preterm birth, low birth weight, and postnatal developmental issues is higher according to research in The Journal of Women’s Health and Pakistan Journal of Biological Sciences.
The most common cause of hypothyroidism in reproductive aged women is Hashimoto’s Disease, an autoimmune condition. The presence of thyroid autoantibodies is used to diagnose autoimmune thyroid reactions. British researcher’s, May 2011 meta-analysis proves that when these thyroid autoantibodies are present, the rates of miscarriage, preterm birth and neurodevelopmental issues are higher, even when thyroid function appears normal by other tests (British Medical Journal). Thus, the American Thyroid Association recommends screening every 4-6 weeks for women with thyroid autoantibodies, even in the absence of disease, due to the increased risk for developing hypothyroidism during pregnancy.
Healthy Adrenals are Important for Healthy Thyroid
It’s important to realize that not all thyroid issues originate with the thyroid. Adrenal dysfunction will influence thyroid function (that spiderweb again…). Thus, treating the thyroid without providing adrenal support may not be productive. The adrenal glands sit on top of the kidneys and mediate the body’s multiple responses to all forms of stress. To do this, adrenals secrete hormones such as cortisol, adrenaline and noradrenaline that act on multiple body systems including nervous, muscular, immune, and cardiovascular. The link between adrenal and thyroid function was recognized decades ago based in part on the coexistence of adrenal diseases with thyroid disorders (King’s College Hospital Medical School, London).
Poor eating habits, a busy schedule, emotional stress, caffeine, food intolerance, immune disorders and other triggers contribute to adrenal stress, with elevated levels of stress hormones such as cortisol being produced. Adrenal stress may manifest in fatigue, mood disturbances, reduced immunity, insomnia, cravings, blood sugar imbalances, and other problems. It also manifests in thyroid imbalances through various mechanisms. For instance, excess cortisol influences hypothalamus and pituitary function in part by altering TRH release by the hypothalamus. Remember that TRH tells the pituitary to make TSH, which tells the thyroid to make thyroid hormone. Adrenal stress also reduces the conversion of T4 to active T3 in target cells and may even decrease the activity of receptor sites on the thyroid that are important for production of thyroid hormone.
If adrenal stress continues long term, adrenal fatigue will eventually develop such that the adrenals no longer make sufficient levels of cortisol and other hormones to meet the body’s needs. Adrenal insufficiency has been linked to subclinical hypothyroidism according to research out of the University of Alabama School of Medicine, and also to increased incidence of autoimmune thyroid reactions like Hashimoto’s (Hormone and Metabolic Research).
Getting Your Thyroid in Shape for Conception and Pregnancy
With the link between hypothyroidism and reproductive fitness, it’s important to support thyroid health directly and also indirectly through supporting adrenal and immune system health before trying to conceive.

Learn How To Support Your Thyroid Naturally With My Thyroid Mini-Course
- Learn how to support your thyroid naturally with nutrition, supplements and plants.
- Know how to tell whether your thyroid, endocrine system or/and adrenals needs support
- Self-care therapies to support your thyroid and endocrine system
Medical Treatment of Hypothyroidism
The American Thyroid Association recommends treatment with levothyroxine (T4) for hypothyroidism regardless of the cause. The problem is that T4 alone is unlikely to help women whose symptoms are due to inefficient conversion of T4 to T3, or from production of elevated levels of rT3. Because of this, many opt for an approach that provides both T3 and T4. Also, if the adrenals are not healthy, this will simply continue to add fuel to the fire.
Nutrition and Hypothyroidism
Focus on nutrient dense, anti-inflammatory foods, with the majority of the diet being a variety of colorful vegetables and fruits, augmented with a smaller amount of healthy proteins, fats and whole grains. The following are some of the key nutrients important for thyroid health. These can be provided by good quality supplements but you should always strive to get as much as possible from food.
Iodine: Iodine is necessary for the production of thyroid hormone and is important for fetal and early postpartum development. Dietary iodine requirements are higher in pregnancy because the demand for T4/T3 is higher and it’s not unusual for iodine levels to drop through pregnancy. Studies have shown that the children of women with mild-to-moderate iodine deficiency (urinary iodine concentrations between 50-150ml/L) during pregnancy are at increased risk for neurodevelopmental issues. The U.S. Institute of Medicine has set the RDA for iodine in pregnant women at 220 μg and 290 μg during lactation, while the RDA for non-pregnant women is 150μg. Be careful not to over-supplement with iodine as it can actually lead to hypothyroidism in susceptible women.
Food sources: Seaweed, seafood, organic dairy, eggs, strawberries.
Selenium: Selenium is important for the function of several enzymes involved in thyroid function. Moreover, selenium has been found to diminish thyroid autoantibody levels. Selenium levels may be low in some pregnant women, and low selenium levels may be a contributing factor to the postpartum thyroid dysfunction that afflicts many women. The RDA for pregnancy is 60 mcg. There is some evidence that long term supplementation with higher levels (200mcg) may contribute to the development of type 2 diabetes.
Food sources: Organic lean meat, fish, Brazil nuts, cheese, eggs, nutritional yeast, liver, butter, cold water fish, alliums (onions, garlic, leeks, etc), mushrooms, tomatoes, green vegetables.
Zinc: Zinc may be involved in many aspects of thyroid function and is both influenced by and influences the thyroid. Make sure your whole food multivitamin contains the RDA for pregnancy, which is 11mg.
Food sources: Organic lean red meat, cheese, duck, goose, turkey, herring, Brazil nuts, pumpkin seeds, whole grains, cucumbers, watermelon rind, peas, carrots, beets.
L-Tyrosine: This is used in the synthesis of thyroid hormone. Should you choose to supplement with L-Tyrosine, be sure not to over-supplement and please talk to your doctor before using it as a supplement if you are taking thyroid hormone.
Supportive foods: Eggs, seaweed, fish, organic poultry, organic pork, game meats, beans, sesame seeds, pumpkin seeds. This may be best from food.
Omega 3 essential fatty acids: These decrease inflammation and support balanced immune system function. Infants born to women with insufficient omega 3 levels are at increased risk for nerve and vision problems. Fish-derived is more bioavailable than flax-derived. The International Society for the Study of Fatty Acids and Lipids recommends 300 mg of DHA daily for pregnancy. DHA is a fish-derived omega 3. Be picky about brand: Poor quality fish oils are actually damaging rather than beneficial.
Food sources: Cold water fish such as salmon, herring, sardines, anchovies, mackerel, trout. Avoid larger fish like tuna that bio-accumulate high levels of mercury.
Vitamins E, C and A: These vitamins are powerful antioxidants, are anti-inflammatory and also immune supporting. The daily recommendations for pregnancy from the Linus Pauling Institute: A (770mcg), C (85mg), E (15mg).
B vitamins: Vitamin B12 deficiency is common in women with hypothyroidism (Journal of Pakistan Medical Association). It is best to get the full range of B vitamins to prevent B vitamin imbalances by taking a vitamin B complex. A good quality fertility-specific, whole foods-based multi will provide the RDA for B complex.
Food sources: Organic meat & poultry, fish, brewerʼs yeast, dairy, eggs, nuts (buy in shell, refrigerated), sunflower seeds, sesame seeds, whole grains, asparagus, spinach, sweet potatoes, avocados, bananas, dried apricots, dates, figs, lentils, beans, peas.
Click here to learn more about a nutritional and herbal supplement for thyroid health…
What to Avoid
- Overeating – May contribute to autoimmune thyroid disorders
- Wheat gluten – Research suggests that Celiac Disease, an autoimmune disorder related to wheat gluten in the diet, has the potential to trigger autoimmune thyroid reactions. Gluten is inflammatory due to the difficulty in digesting it.
- Other inflammatory foods – Processed or damaged fats, alcohol, sugar, processed flour.
- Excess salt – Another potential contributing factor to autoimmune reactions
- Soy – May inhibit thyroid function
- Flaxseeds – May inhibit thyroid function
- Raw cruciferous vegetables (eg. Broccoli, cauliflower, kale, cabbage, etc. Cooked are OK) – May inhibit thyroid function
Herbal Support
The best time for herbal support is in preparation for conception. Talk to your doctor before using any supplements if you are taking thyroid hormone.
Maca (Lepidium meyenii) – A nourishing superfood that supports pituitary, thyroid, adrenal and reproductive function. More information here…
Vitex (Vitex agnus-castus) – Endocrine support via actions on the pituitary gland. Primary effects are on the ovaries, but it may provide thyroid and adrenal support as well. More information here…
Asian Ginseng (Panax ginseng) – An adaptogen (influences hypothalamus and pituitary function to increase stress resistance). Also it is an adrenal and reproductive tonic while stimulating thyroid function. This herb is best for seriously debilitated folks and is not appropriate for those under the age of 40. It may be overstimulating otherwise.
Eleuthero (Eleutherococcus senticosus) – An adaptogen and adrenal tonic. It may be overstimulating for some people, but is less stimulating overall than Asian Ginseng.
Ashwagandha (Withania somnifera) – An adaptogen, adrenal tonic, reproductive system tonic and thyroid stimulant. Because it is an immunomodulator that may modulate the body’s inflammatory responses, it is used for support with Hashimoto’s Disease. May help with stress-related infertility.
Schisandra (Schisandra chinensis) – Adaptogen, adrenal tonic and immunomodulatory herb with thyroid stimulating activity. Used for support in Hashimoto’s. Supports liver health and may help with stress-related infertility.
Rhodiola (Rhodiola rosea) – Another adaptogen and adrenal tonic that provides reproductive system support.
Licorice (Glycyrrhiza glabra) – An adaptogen and adrenal tonic that also contains phytoestrogens that may balance the body’s estrogen activities. It is also an immunomodulator. Also provides liver support. Healthy liver function is required for hormonal balance.
Guggal (Commiphora mukul) – Ayurvedic tonic that supports T4-T3 conversion and healthy reproductive function.
Milky Oat Tops (Avena sativa, A. fatua) – Supports thyroid function and is a nourishing adrenal tonic that also supports nervous system.
Gotu Kola (Centella asiatica) – Supports thyroid function. Has been used for support in Subclinical Hypothyroidism. May support improved FSH and LH production in low thyroid function. Note: It can be hard to get good quality Gotu Kola, be sure to purchase from a reputable source.
Seaweed – A good source of minerals, including iodine. Don’t overdo, as too much iodine will suppress rather than support thyroid function. The iodine in seaweed may protect the thyroid from radioactivity.
Closing Thoughts
It is absolutely vital for women who have been struggling to conceive, have experienced 2 or more miscarriages or suspect a thyroid issue to get proper testing prior to trying to conceive. Request that your doctor run a full thyroid hormone panel for proper diagnosis. Support thyroid health and total body wellness through key foods, nutrients and herbs shown to positively impact thyroid health and the entire endocrine system. Work closely with your doctor to ensure thyroid hormone levels are stable enough to sustain a healthy pregnancy. Continue to have your thyroid levels monitored and adjusted if needed throughout pregnancy and breastfeeding.
Click here to learn more about a nutritional and herbal supplement for thyroid health…
Too learn more about related subjects covered in this article, please visit the following links:
Is My Adrenal Health Affecting My Fertility?
Cod Liver Oil Essential for Healthy Fertility and Pregnancy
Celiac Disease Increases Risk of Infertility
- Arafah, BM (2001) Increased need for thyroxine in women with hypothyroidism during estrogen therapy. N Engl J Med. 344(23):1743-9. Retrieved from: https://www.nejm.org/doi/full/10.1056/NEJM200106073442302
- Acharya, N (2011) Gonadotropin levels in hypothyroid women of reproductive age group. J Obstet Gynaecol India. 61(5):550-3. Retrieved from: https://link.springer.com/article/10.1007/s13224-011-0079-7
- Sharma, Y et al (2006) Ovarian cysts in young girls with hypothyroidism: follow-up and effect of treatment. J Pediatr Endocrinol Metab.19(7):895-900. Retrieved from: https://www.degruyter.com/view/j/jpem.2006.19.7/jpem.2006.19.7.895/jpem.2006.19.7.895.xml
- Stagnaro-Green, A. et al (2011) Guidelines of the American Thyroid Association for the Diagnosis and Management of Thyroid Disease During Pregnancy and Postpartum. Thyroid. 21(10):1081-1125. Retrieved from: https://www.liebertpub.com/doi/10.1089/thy.2011.0087
- Mansourian AR (2013) Female reproduction physiology adversely manipulated by thyroid disorders: a review of literature. Pak J Biol Sci. 6(3):112-20. Retrieved from: http://docsdrive.com/pdfs/ansinet/pjbs/2013/112-120.pdf
- Galofre, JC and TF Davies (2009) Autoimmune thyroid disease in pregnancy: A review. Journal of Women’s Health. 18(11):1847-56. Retrieved from: https://www.liebertpub.com/doi/full/10.1089/jwh.2008.1234
- Thangaratinam S, et al (2009) Association between thyroid autoantibodies and miscarriage and preterm birth: meta-analysis of evidence. BMJ. 342:d2616. Retrieved from: https://www.bmj.com/content/342/bmj.d2616
- Parsons, V. and I. Ramsey(1968) Thyroid and adrenal relationships. Postgrad Med J. 44:377-84. Retrieved from: http://europepmc.org/backend/ptpmcrender.fcgi?accid=PMC2466598&blobtype=pdf
- Abdullatif, HD and AP Ashraf (2006) Reversible subclinical hypothyroidism in the presence of adrenal insufficiency. Endocr Pract. 12(5): 572. Retrieved from: http://journals.aace.com/doi/abs/10.4158/EP.12.5.572
- Legakis, I, et al (2001) Elevated prolactin to cortisol ratio and polyclonal autoimmune activation in Hashimoto’s thyroiditis. Horm Metab Res. 33(10):585-9. Retrieved from: https://www.thieme-connect.com/products/ejournals/abstract/10.1055/s-2001-17904
- Duntas, L. and D. Micic (2012) Adiposopathy and thyroid disease: tracing the pathway to cardiovascular risk. Expert Rev Cardiovasc Ther. 10(6):797-803. Retrieved from: https://www.tandfonline.com/doi/abs/10.1586/erc.12.47?journalCode=ierk20
- Jabbar, A., Yawar, A., Waseem, S., Islam, N., Ul, N., Zuberi, L., . . . Akhter, J. (2008, May). Vitamin B12 deficiency common in primary hypothyroidism. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/18655403
- Duntas, L (2009) Does celiac disease trigger autoimmune thyroiditis? Nat Rev Endocrin. 5(4):190-1. Retrieved from: https://www.nature.com/articles/nrendo.2009.46
- Jabbar A, Yawar A, Waseem S, Islam N, Ul Haque N, Zuberi L, Khan A, Akhter J. J Pak Med Assoc. 2008 May;58(5):258-61. Vitamin B12 deficiency common in primary hypothyroidism. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/18655403
- Shomon, Mary J. (2006) The Thyroid Hormone Breakthrough. HarperCollins.





