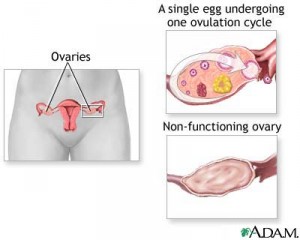
 Premature Ovarian Failure (POF), also known as Ovarian Hypofunction, is defined as a loss of normal ovarian function before the age of 40. Some people think that POF is premature menopause, but menopause is a natural process the female body goes through as it ages. During menopause, a woman’s body will gradually, over many years, stop producing mature follicles (eggs) for ovulation. Estrogen and progesterone levels naturally decline causing the menstrual cycle to come less often until eventually it stops. The normal age range for women to naturally go through menopause is 45-55, with the average mean age of 51.
Premature Ovarian Failure (POF), also known as Ovarian Hypofunction, is defined as a loss of normal ovarian function before the age of 40. Some people think that POF is premature menopause, but menopause is a natural process the female body goes through as it ages. During menopause, a woman’s body will gradually, over many years, stop producing mature follicles (eggs) for ovulation. Estrogen and progesterone levels naturally decline causing the menstrual cycle to come less often until eventually it stops. The normal age range for women to naturally go through menopause is 45-55, with the average mean age of 51.
Unlike menopause, POF is not a naturally occurring process for a woman’s body. There are different reasons a woman may be diagnosed with POF; these are broken down into two categories: follicle dysfunction and follicle depletion.
Throughout a woman’s life her ovaries contain thousands of follicles, and these follicles contain eggs. The pituitary gland begins releasing FSH at the beginning of the menstrual cycle and the release of FSH signals some of the follicles in the ovary to mature. As the follicles begin to mature they are supposed to release estrogen over time. The rising estrogen level signals the pituitary gland to curb the release of FSH. If the follicles do not mature (and thus do not produce enough estrogen; the low estrogen signals the pituitary to crank out more FSH) and the FSH levels remain high. Women with POF show high levels of FSH. This is why the doctors perform FSH tests, to see if the levels are too high. In a normal functioning follicle, the estrogen levels rise and signal the pituitary gland to release Lutenizing Hormone (LH). LH signals the follicle to open and release the mature egg at ovulation and produces progesterone to ripen the uterine lining for implantation. When the delicate communication between the pituitary gland, the ovaries and the follicles does not work properly, ovulation does not occur.
Let’s look at different reasons POF may happen under those categories.
Follicle Dysfunction
Follicle dysfunction happens when your follicles are not responding properly. Here are some possible causes…
Autoimmune Disorders: An autoimmune disease happens infrequently, but is on the rise. Autoimmune diseases in some cases may damage follicles; by the woman’s body producing antibodies that attack the ovaries and in turn may harm and damage the follicles. Doctors are not sure why this occurs, but some say it may be due to an exposure to a virus. When a follicle becomes damaged it can no longer produce estrogen properly which is the key hormone it releases to communicate with the pituitary gland.
The use of Systemic Enzymes may prove effective in helping with autoimmune disorders.
Follicle Depletion: This is defined as low or few follicles responding to the signal of the FSH being released. These follicles still exist in the body, they just don’t communicate. Over time they begin to die off and diminish as the entire reproductive system begins to suffer. The communication and proper function of the reproductive system is fragile and is one that depends on all of its parts to operate accurately to maintain vitality. If the follicles do not mature, ovulation stops happening and the menstrual cycle becomes irregular or stops completely because there is no estrogen and progesterone to make a uterine lining to shed.
Causes of follicle depletion
- Environmental toxins including pesticides, herbicides, cigarette smoke, pollutants, chemicals
- Exposure to a virus
- Chromosomal defects, including Turner’s Syndrome and X syndrome
- Genetic predisposition, this may run in some families, accounting for 10% of POF cases
- Chemotherapy and radiation treatments are some of the leading causes of POF and follicle depletion
While we cannot control genetic factors, or situations where we have had to make hard decisions like choosing chemotherapy or radiation to fight other health problems, we can work toward avoiding toxins. Here are some tips for avoiding toxins…
2. Avoid using pesticides or herbicides in your yard, garden or surrounding areas.
3. Avoid synthetic-chemical-loaded-mainstream body products including make-up.
4. Avoid using feminine products that are not made from organic cotton, contain plastic or are made from rayon.
5. Drink filtered water, avoid tap water.
Symptoms of POF
Symptoms of POF are similar to those of menopause, but may be more extreme.
- Irregular periods (Note: other conditions such as PCOS also have this symptom)
- Night sweats
- Hot flashes
- Brain fog – inability or difficulty in focusing
- Irritability
- Vaginal dryness
- Unexplained infertility
- Low libido
All of these symptoms are similar to other fertility issues, which makes self-diagnosis incredibly difficult. If you have missed your period for over 3 months and are over the age of 35, you may want to talk to your doctor about testing for POF. I don’t want to scare any of you, but it is important when dealing with fertility issues to have a good solid diagnosis so that you can know where to go from there; a starting point and options.
How is POF Diagnosed?
POF is usually diagnosed by having your estrogen and FSH levels tested. Extremely low levels of estradiol (estrogen) and high levels of FSH are signs that the ovarian follicles are no longer responding to the FSH to increase estrogen levels. AMH or anti-mullerian hormone may be tested as well especially if you desire to become pregnant.
Ultrasound imaging may be helpful in that it can show if the ovary is the right size and shape. This kind of scan may help to see the follicle count and if the ovary is atrophied.
There is also a blood test that measures the levels of AMH (Anti-Mullerian Hormone) also known as MIS ( Mullerian Inhibiting Substance) which is produced directly by the follicles. AMH levels correlate with how many antral follicles are in the ovaries. Women with low levels of AMH typically have low levels of follicles.
What if I have already been diagnosed with POF?
First off, I would like to say that my heart goes out to you, as this can be a devastating diagnosis. It is pretty much a consensus across the board that POF is a difficult condition to properly diagnose. If you have already been given a diagnosis of POF it is important to have clear communication with your doctor about the tests you have been given for this conclusion. A definitive diagnosis of POF usually means that you will have extreme difficulty getting pregnant; though women with POF may still become pregnant. So, do not give up hope if you have not yet had a child because it could still happen.
Natural Ways to Support the Body In the Prevention of Premature Ovarian Failure
Remember, these will only help in supporting the body’s natural functions and cannot cure POF or prevent POF from happening if there is a genetic factor or chromosomal defects. Focusing on Improving Egg Health, nourishing the endocrine system and maintaining optimum health of the ovaries, fallopian tubes and uterus are vital. Below are some ways to support all of these important parts of fertility.
Natural Fertility Diet
Nutrition plays a big role when it comes to having a healthy body and reproductive system. The building blocks for hormones are found in the foods we eat. Antioxidants which help to protect the eggs and tissues of the reproductive system are found in the foods that we eat. What we eat each day is the foundation for our health and those foods have a great impact on our fertility. Eating a whole foods based fertility diet is the first step to helping the body and your fertility function at its best.
Maca
Maca is a nourishing food for the endocrine system, aiding the pituitary, adrenal, and thyroid glands (all involved in hormonal balance). This superfood works to protect the body from the damaging effects of stress, supports egg health and has been shown to increase libido.
Shatavari
Shatavari is an Indian herb that has been used for thousands of years in the healing practice of Ayurveda. Its main constituent is steroidal saponins, giving rise to the conclusion that Shatavari has the ability to act as an estrogen modulator that may help regulate the menstrual cycle. This herb has adaptogenic and immuno-modulating properties, meaning it may be helpful with women who have stress related or immune-mediated fertility issues.
Vitex
Vitex supports hormonal balance in the body by having an effect on the hypothalamic-pituitary-ovarian axis (hormonal feedback loop), correcting the problem at the source. Vitex, also known as chaste tree berry, is usually the first line of defense in a woman who is experiencing irregular periods, helping to regulate communication of the entire reproductive system.
Royal Jelly
Regular consumption of high-quality Royal Jelly has been shown to help balance hormones. This makes it beneficial to those individuals that suffer from a hormonal imbalance, as it helps to provide support to the endocrine system. It can also help with problems that are related to hormonal imbalance, such as polycystic ovarian syndrome or irregular menstrual cycles. Some studies have shown that Royal Jelly has the propensity to mimic human estrogen, which can help those who suffer from low estrogen levels. Royal Jelly is rich in amino acids, lipids, sugars, vitamins, and most importantly, proteins. It contains high levels of vitamins D and E, and also has ample levels of iron and calcium, all of which are essential to proper health and organ function.
Systemic Enzyme Therapy
Systemic enzymes have been shown to greatly reduce an over-active immune response which is when antibodies attack with the intent to destroy our own tissues or that of another person’s (sperm or a fetus).
Self Fertility Massage
This type of massage may promote hormonal balance by strengthening the hormonal feedback loop, increasing circulation to the uterus, ovaries, and fallopian tubes, bringing fresh, oxygenated, and nutrient-rich blood to the eggs, improving uterine tone, as well as aiding in the body’s elimination of toxins. Self-Fertility Massage can be performed on yourself in the comfort of your home.
Exercise
A sedentary, inactive lifestyle does not promote an environment to naturally cleanse the body of excess hormones and toxins. Exercise gets our hearts beating faster which in turn pumps more fresh oxygenated blood to the entire body; mainly our vital organs – each playing a vital role in our body functioning properly. This increase in circulation also helps with the elimination of toxins. Additionally, exercise increases body temperature triggering the sweat glands to produce sweat to cool us down. Sweat is another way our bodies remove toxins. Exercise at least 30 minutes a day, 5 times a week.
Closing Thoughts
It is never too late to begin to think about the future of our health. Premature Ovarian Failure shows us how intricately connected our reproductive system is connected with our brain and entire body and how environmental toxins play a huge role in infertility. Now is the time to work toward supporting the entire body’s health for the future by supporting its natural functions through diet, exercise, clean water and supportive natural therapies. Premature ovarian failure (POF) is a perplexing fertility health diagnosis that leaves women feeling heartbroken. Find hope and keep moving forward by Nurturing Yourself & Your Fertility With POF.
- Premature Ovarian Failure (POF). (n.d.). Retrieved from: https://resolve.org/infertility-101/medical-conditions/premature-ovarian-failure/
- Mayo Clinic. (2008). Premature Ovarian Failure. Retrieved from: http://www.mayoclinic.com/health/premature-ovarian-failure/DS00843
- Loes. M. M.D.(H.). (2010). The New Aspirin Alternative – The natural way to overcome chronic pain, reduce inflammation and enhance the healing response. Freedom Press.
- Jankowska, K. (2017). Premature ovarian failure. Menopausal Review, 2, 51-56. doi:10.5114/pm.2017.68592 Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5509972/
- Romm, Aviva. (2010). Botanical Medicine for Women’s Health. St. Louis, Missouri: Churchill Livingstone.





